The most dangerous part of “the drug that could end obesity” isn’t the medicine—it’s the certainty.
Quick Take
- GLP-1 and newer dual- and triple-agonist drugs can drive 10–16% (and sometimes more) weight loss, but they do not “cure” obesity.
- The market has shifted from older stimulants and mixed-effect pills to powerful hormone-mimicking therapies that change appetite and metabolism.
- Oral versions and next-generation compounds are racing through trials, aiming to match injections and reduce side effects.
- Black-market peptides and unregulated “research” vials create real safety risks that hype rarely mentions.
The Viral Hook Meets a Very Real Medical Revolution
“This Drug Could End Obesity?!” works as a headline because it whispers what millions want to believe: that biology finally has an off-switch for hunger and weight gain. The more honest takeaway lands differently. New obesity medicines can overpower appetite signals for long stretches, but they don’t erase the underlying tendency to regain weight when treatment stops. That gap between hope and reality is where social media thrives—and where bad decisions begin.
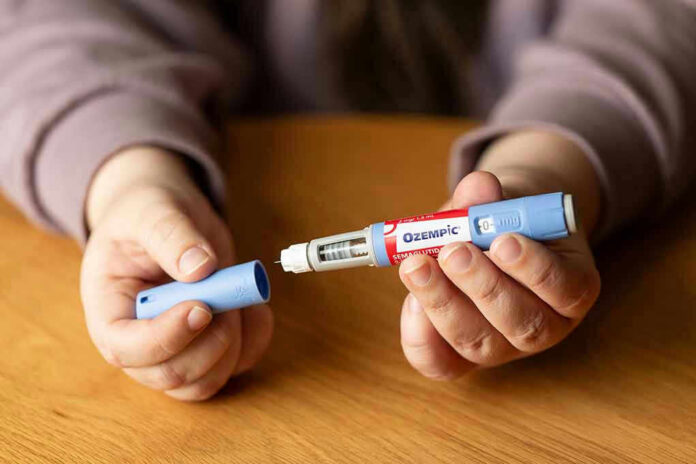
GLP-1 medications started as diabetes treatments and then collided with the modern obesity crisis. They slow gastric emptying, curb appetite, and improve glucose control—effects that can feel “miraculous” to people who have fought cravings and scale creep for decades. When you see consistent double-digit percentage losses reported, it’s easy to jump to absolutes. Medicine rarely rewards absolutes; it rewards monitoring, dosing discipline, and long-term follow-through.
How Weight-Loss Drugs Evolved From Blunt Tools to Precision Hormones
Obesity pharmacology has a long memory, and it isn’t sentimental. Earlier options leaned on appetite suppression or combinations that delivered modest average reductions but came with tradeoffs. Some drugs left the market after safety concerns; others remained but never broke through public skepticism. The GLP-1 era changed the conversation because the average outcomes started to look like something closer to a surgical result—without surgery—at least on paper.
Semaglutide’s rise and tirzepatide’s entrance accelerated the “war on obesity” narrative and created a new baseline for what patients expect. People who once celebrated five percent weight loss now ask about fifteen or twenty. That shift matters: higher expectations can motivate healthier behavior, but they also create a consumer mindset where the drug becomes the plan. Obesity responds better when the drug supports a plan, not when it replaces one.
The Next Wave: Orals, Multi-Agonists, and a Race to Beat Side Effects
Drug developers aren’t just chasing more weight loss; they’re chasing better weight loss with fewer compromises. Orals aim to remove the weekly injection barrier and widen adoption. Multi-agonists—drugs that act on more than one metabolic receptor—aim to push results while improving tolerability or reducing the loss of lean mass that can accompany rapid weight reduction. Trial headlines now compete on percentage points the way car companies compete on horsepower.
Phase 2 results for newer oral candidates have drawn attention because they suggest double-digit loss might not require a syringe. That has enormous implications for access and adherence, but it also raises the stakes for proper prescribing. A pill feels casual; these drugs are not casual. Even when trials look strong, real-world use includes missed doses, cost-driven interruptions, and people trying to “hack” treatment without medical supervision—all of which can blunt benefits and amplify risk.
What the Hype Leaves Out: Obesity Is Chronic, and So Is the Management
“End obesity” language usually skips the most conservative, common-sense reality: chronic conditions often require chronic management. Many patients regain weight after discontinuation, which doesn’t mean the drug “failed”—it means the biology reverted when the signal changed. That pattern mirrors hypertension and high cholesterol more than it mirrors an infection cured by antibiotics. The durable win comes from treating obesity as a long-term medical issue, not a short-term vanity project.
Side effects also deserve adult conversation. Gastrointestinal issues remain common. Rapid losses can include lean mass, which matters to readers over 40 who already fight age-related muscle decline. The future of the category likely belongs to regimens that protect function: preserving strength, improving glucose markers, and reducing cardiovascular risk while keeping weight off. The scale number is loud; health outcomes are the point.
The Black-Market Peptide Trap That Follows Every “Miracle” Narrative
Whenever a therapy becomes culturally iconic, a shadow market follows. Peptides advertised online as “research only” or sold through unauthorized channels can tempt people priced out of brand-name prescriptions or tired of waiting for supply. That’s where the viral story’s warning matters. Unregulated products can be mislabeled, contaminated, improperly stored, or incorrectly dosed. Buyers also lose the clinical guardrails: screening, titration schedules, and monitoring for adverse effects.
American conservative values tend to favor personal responsibility and informed consent, and those principles cut against DIY pharmacology. People should have the freedom to pursue better health, but freedom works best when paired with transparency and legitimate oversight. If a product’s origin, dosing accuracy, and quality controls can’t be verified, the “savings” can become a medical bill—or worse. No headline is worth gambling on what’s inside a mystery vial.
This Drug Could End Obesity?! 🤯
Continue watching the FULL episode with Louisa Nicola at 12:30 PM CST.@louisanicola_ pic.twitter.com/x1bT3vFwrj
— Shawn Ryan Show (@ShawnRyanShow) April 30, 2026
The smarter way to read the “end obesity” claim is as a signal: the science is improving fast, and the business incentives are enormous. Novo Nordisk and Eli Lilly are fighting for dominance, while smaller biotechs chase oral options and new mechanisms. That competition can benefit patients, but it also rewards sensationalism. Treat the drug as a tool, treat obesity as chronic, and treat unregulated shortcuts as the risk they are.
Sources:
New Weight-Loss Drugs: What’s Coming and What’s Available
Pharmacological Treatment of Obesity: A Review